SPECIAL REPORT: ‘Every life lost impacts us all’
Indiana has one of the highest infant mortality rates in the nation. Now regional healthcare is evolving to address families' needs.

At age 24, Cassius Stallings has invested in the south side of Fort Wayne his entire life.
He graduated from South Side High School, worked for Youth for Christ, and even worked at the Walmart on Southtown Crossing Blvd. near his house.

Then, about six months ago, he found a new way to get involved.
He heard that Parkview Health was hiring community health workers to go out into neighborhoods on the southeast side and work with moms and babies to help reduce northeast Indiana’s infant mortality rate (IMR).
As a whole, Indiana has the eighth-highest infant mortality rate in the nation. In 2016, 623 babies died before their first birthday—including 80 in northeast Indiana alone.
Since Stallings recently became a father himself, the statistics moved him to action.

“It really hit me: This is serious,” Stallings says. “It could have been my son.”
Today, after six months on the job, he is one of Parkview’s first community health workers as part of a program designed to turn the traditional model of prenatal services upside-down, says Erin Norton, Director of Community Outreach for Parkview’s Women and Children’s Service Line.
For 20 years, Parkview’s Integrated Community Nursing Program has sent RNs into homes to work with residents where they are. Now Stallings and other community health workers are coming alongside these nurses to serve residents, too, and instead of being experts on medical information, they’re experts on people and places.
“Traditionally the model has been that you bring in your doctor or your nurse who is an expert on the content area, and you filter down the information,” Norton says. “We’ve kind of switched that paradigm by finding people who are experts in the community and providing them with specific education about topics that affect moms and babies.”

The idea is to create a self-sustaining network of support in communities where infants are dying most often, starting in the 46805 and 46806 zip codes, then expanding to all of Fort Wayne, and eventually all of northeast Indiana.
It’s part of an encouraging trend Norton has seen in her time working with moms and babies across the region.
Instead of blaming mothers or families for infant deaths, communities are taking responsibility to help them because in the same way it takes a village to raise a child, it also costs a village to lose one.
“While infant mortality is sometimes seen as a heartbreak for an individual family, which it certainly is, it also should be a heartbreak for the whole community,” Norton says. “Every life lost impacts us all.”
***
By definition, a population’s infant mortality rate is the number of babies who die before their first birthday, per 1,000 live births.
Although the United States is one of the most developed countries in the world, it also has one of the world’s highest IMRs at 5.8, more than 2 points over the comparable country average.
Indiana and northeast Indiana are no exception, with IMRs of 7.6 and 7.8, respectively.
And beyond the emotional distress caused by babies dying, there are economic effects, too.

Across the country, having a high IMR places a multibillion-dollar burden on business, with employers billed more than $12 billion annually in excess healthcare costs.
As a result, Indiana Governor Eric Holcomb has proposed making Indiana the state with the lowest IMR in the Midwest by 2024.
To accomplish this, the state Department of Health has developed a comprehensive strategy and set aside $11 million to fund competitive grants to support programs addressing the issue.
In 2017, Parkview was awarded $3.6 million from that fund through the Safety PIN (Protecting Indiana’s Newborns) grant to combat the IMR in Allen County. This grant has allowed them to launch the community health worker program free of cost to participants.

So far, Parkview has hired four community health workers, including Stallings, and they expect to hire six more by the end of the year.
Norton says another vital part of the program’s success is its partnerships with regional groups that have similar missions, like the St. Joseph Community Health Foundation, the African-American Healthcare Alliance of Fort Wayne, Health Visions of Fort Wayne, the Fort Wayne Allen County Department of Health, and Chi Eta Phi Sorority, just to name a few.
“Fort Wayne is really fortunate that we have so many organizations working to help moms and babies,” she says. “So one of our primary focuses is going to be directing women we see through outreach into these organizations’ programs.”

But part of the puzzle is getting services to women and families who have no transportation. That’s where the benefits of community health workers come into play.
Workers like Stallings are flexible to meet families’ needs—whether they only want a few tips or need consistent care throughout the week.
Although community health workers go through training to learn the medical side of serving moms and babies, the tasks they are performing often don’t require medical knowledge, Norton says. Instead, they might be helping moms get nutritious groceries or making sure they have transportation to follow up on their doctors’ instructions.
“If you’re a pregnant woman, and let’s say you have gestational diabetes, you’ve gone to the doctor’s office and gotten a lot of education, so you know what you need to do,” Norton says. “But when you get home, you might realize, ‘I don’t know how to get the foods I need. I live in a food desert, and I have to ride a bus an hour to get to a grocery store that sells fresh produce. How am I going to navigate this?’ That’s where a community health worker can come in and help work through those basic barriers.”
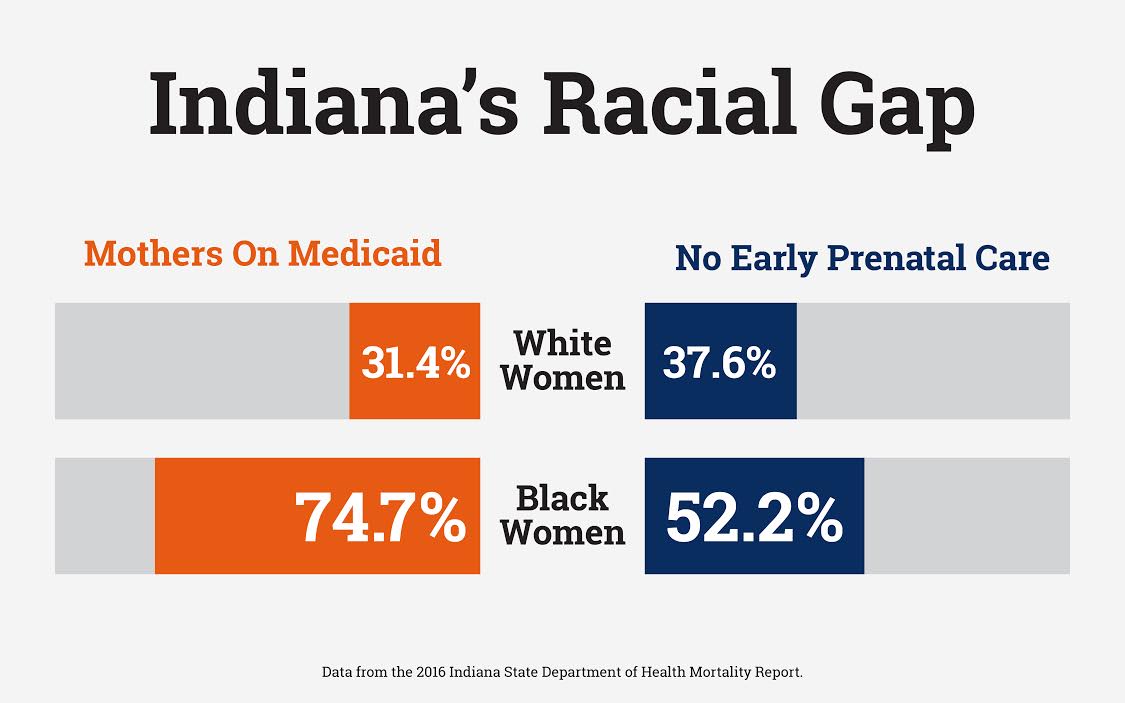
Stats from the Indiana State Department of Health show that helping moms overcome basic barriers to resources like food and transportation could make all the difference. In Fort Wayne and across the nation, the largest cause of infant mortality is babies being born too soon, which is less likely to happen if moms are receiving quality prenatal care, Norton says.
But she explains that, for many moms in northeast Indiana, prenatal care is out of reach.
“Some of these mothers are working two jobs, and going to prenatal appointments is really hard,” Norton says. “Perhaps they’re having to choose between their kids having enough food to eat the next day versus them going to a doctor’s appointment.”
On top of that, the barriers to prenatal care are often higher for moms and babies who aren’t white.
***
In an early blog post about Parkview’s new community health worker program, Patti Brahe, Senior Vice President of Parkview’s Women’s and Children’s Services put it simply: “We have to talk about what this really is, and the truth is, African American babies are dying more than white babies.”

While the IMR in Allen County is 6.6 percent among white babies, it is more than double that figure at 14 percent among African American babies, and for many reasons, Norton explains.
Along with economic inequality and access issues, another potential reason is preterm deliveries caused by stress.
“There’s a lot of new research coming out about how stress plays a role, and it could be an individual stressor or societal stressors,” she says. “I think that’s going to be one of our focuses going forward.”
In the meantime, Stallings says that simply having conversations about racial disparities and barriers to prenatal care can be helpful in the healing process.
“It’s just getting that awareness out there,” he says. “Just having these conversations with people is huge because that speaks value to this situation and understanding that, ‘Ok, there’s people noticing it. Now what can we do to help?’”
Norton agrees and encourages northeast Indiana residents of all races to think and talk about infant mortality more often despite its taboo topics.
“Talking about race can be pretty uncomfortable, and talking about babies dying can be pretty uncomfortable,” she says. “But the problem is too important to let being uncomfortable stand in the way of what needs to be done.”
This Special Report was made possible by Parkview Health.











